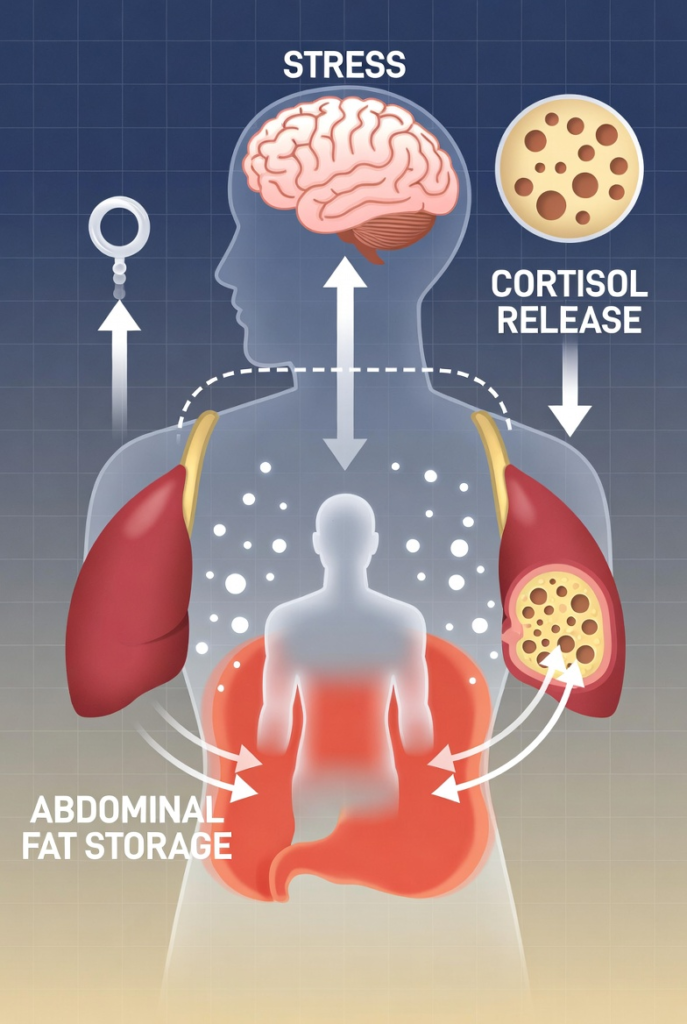
Ever feel like you’re doing “the right things” for weight loss, but your body doesn’t get the memo? You’re eating better, moving more, and still the scale creeps up, especially around your middle. Stress can be a quiet driver here, because it changes how hungry you feel, how you sleep, and how your body handles sugar. The key hormone is cortisol, which is normal and helpful in short bursts. It’s your built-in alarm system.
The problem starts when cortisol stays high for weeks or months. That’s when cortisol and weight gain often start traveling together. Below, you’ll learn how that connection works, then follow a practical 14-day plan to calm cortisol and support a healthier metabolism.
How cortisol can lead to weight gain (even if you are trying hard)
Cortisol is supposed to rise in the morning to help you wake up, then taper off at night so you can sleep. Chronic stress flips that rhythm. So does short sleep, late-night work, endless scrolling, or caffeine that lingers too long.
When your brain thinks danger is near (even if the “danger” is email and bills), cortisol helps you survive. It pushes more fuel into your bloodstream and nudges you to seek quick energy. That makes sense for a short emergency. However, modern stress is rarely short.
Over time, high cortisol can make your body act like it needs to store, not spend. Your appetite changes, cravings get louder, and workouts feel harder to recover from. Many people also move less without realizing it. Small dips in daily movement can erase a lot of gym effort.
A recent report highlighted how often cortisol issues show up alongside stubborn metabolic problems. For example, the Catalyst study described a meaningful subset of people with difficult-to-manage obesity and diabetes who had elevated cortisol patterns contributing to the problem.
If your life feels like one long “urgent” moment, your body may start budgeting calories like it’s preparing for winter.
It changes where your body stores fat, and why belly fat shows up first
With chronic stress, fat storage tends to drift toward the midsection. The “deep” belly fat is called visceral fat, which sits around organs, not just under the skin. Think of it as padding your body adds deeper inside the abdomen.
Why does this matter? Visceral fat is more tied to cardiometabolic risk than the softer, pinchable fat on hips or thighs. It can also make your waistline change even when your weight barely moves. If you keep hearing about “cortisol belly,” this is the idea people are pointing to, although the reality is more nuanced than social media makes it sound. A useful reality check is this breakdown of stress and belly fat myths.
It can raise blood sugar, push insulin up, and make fat storage easier
Cortisol helps release “emergency fuel” by raising blood sugar. That’s helpful if you’re running from a threat. Yet repeated stress spikes can keep blood sugar higher more often.
Your body answers that with more insulin, because insulin moves sugar out of the blood and into cells. When that cycle repeats, some people drift toward insulin resistance. In plain terms, the same amount of insulin doesn’t work as well, so the body makes more. Higher insulin can make fat storage easier, especially around the middle.
It ramps up cravings and makes comfort foods feel extra rewarding
Stress doesn’t just make you “hungry.” It can make you want specific foods: sugary, salty, and high-fat snacks that deliver fast relief. The brain gets a quick reward, then energy drops, and cravings pop back up later.
Poor sleep turns up the volume. After a short night, appetite signals shift, and impulse control tends to dip. That’s why stress eating often feels less like a choice and more like gravity.
It can slow your calorie burn by reducing muscle and daily movement
Long-term stress can chip away at muscle, and muscle helps you burn more calories at rest. At the same time, stress makes many people tired and stiff, so they fidget less, take fewer steps, and skip optional movement.
Extreme dieting can add to the squeeze. When you cut calories hard while you’re stressed and underslept, your body often responds by downshifting energy use and increasing food focus. The result is frustrating: you try harder, and progress slows.
Quick self-check: signs your cortisol is running high (and when to talk to a doctor)
You can’t diagnose cortisol issues by vibes alone. Still, patterns matter. If you see several of these signs together, it’s a clue your stress load and sleep rhythm need attention.
Common clues: sleep trouble, belly weight gain, cravings, and feeling wired but tired
Here are everyday signs people often notice:
- Trouble falling asleep, or waking up around 2 to 4 a.m.
- Feeling tired in the morning, then getting a “second wind” at night
- More belly weight gain than usual, or a growing waistline
- Stronger cravings for sweets, chips, or fast food
- Feeling wired but tired, edgy, or on high alert
- Frequent headaches, tight jaw, or tense shoulders
- More irritability or anxiety than normal
- Workouts feel harder to recover from
If you want a plain-language checklist to compare against, this guide on signs cortisol may be high is a helpful starting point.
Red flags that deserve medical help, not more willpower
Some situations call for a clinician, especially if symptoms are strong or persistent. Talk to your doctor if you have:
- Ongoing high blood pressure readings
- Blood sugar issues, or new prediabetes or diabetes concerns
- Rapid, unexplained weight change
- Severe fatigue, mood changes, or depression that isn’t improving
- Use of corticosteroid medications (pills, injections, high-dose inhalers)
- Symptoms that keep worsening, or don’t improve with sleep and stress changes
Rarely, a condition like Cushing syndrome can drive very high cortisol. It’s uncommon, but it’s one reason not to self-blame.
A 14-day reset plan to calm cortisol and support your metabolism
This isn’t a crash diet. Think of it like resetting a smoke alarm that’s too sensitive. The goal is fewer false alarms, so your metabolism can run normally again.
Track just one or two metrics for two weeks: average sleep hours, waist measurement, or a daily cravings score from 1 to 10. Small data beats guesswork.
Here’s a simple structure for the 14 days:
| Days | Main focus | What you’re aiming for |
|---|---|---|
| 1 to 4 | Sleep and morning light | Restore your cortisol rhythm |
| 5 to 8 | Steady meals | Fewer blood sugar swings |
| 9 to 12 | Movement that feels good | More steps, better recovery |
| 13 to 14 | Stress tools | Less reactivity, better choices |
Start with sleep and timing, because cortisol follows a daily rhythm
First, pick a consistent wake time, even on weekends. Then work backward to get 7 to 9 hours in bed. Next, get outside light within an hour of waking for 5 to 10 minutes.
Keep caffeine earlier, ideally stopping by late morning or early afternoon. In the evening, dim lights and build a short wind-down routine (shower, stretch, book, same order). Finally, make your room cool and dark.
Nighttime cortisol spikes can make weight management harder, because they wreck sleep and push next-day cravings.
Eat to steady blood sugar: protein at breakfast, fiber at meals, fewer sugar hits
Start the day with protein, because it can smooth hunger later. Aim for a protein plus fiber anchor at each meal, for example eggs plus fruit, Greek yogurt plus berries, chicken plus beans, tofu plus vegetables.
Don’t force a skipped breakfast if it leads to late-day grazing. Instead, choose a simple first meal you can repeat. Keep sweets and ultra-processed snacks as “sometimes” foods, not daily stress medicine.
Helpful foods aren’t magic, but they support the plan: omega-3-rich fish, magnesium-rich greens and beans, and fermented foods like yogurt or kimchi. A sample day can be as simple as eggs and spinach at breakfast, a turkey and bean salad at lunch, and salmon with roasted veggies and rice at dinner.
For more symptom context and practical lifestyle ideas, see Verywell Health’s overview of cortisol belly causes and solutions.
Move in a way that lowers stress, not spikes it all day
Walking is underrated. A 10 to 20-minute walk, especially after meals, helps burn off stress energy and supports blood sugar control. Add strength training 2 to 3 times per week to protect muscle.
Hard workouts can raise cortisol short term, and that’s not “bad.” Still, if you’re already running on fumes, going all-out daily can keep you in recovery debt. Build in easier days and finish sessions feeling like you could do a little more.
Beginner weekly template: two short strength sessions, two longer walks, and daily 10-minute walks when you can.
Use 5-minute stress tools that work when life is busy
Stress skills work best when they’re small and repeatable. Try one tool twice a day for two weeks.
Box breathing (inhale 4, hold 4, exhale 4, hold 4) or simply longer exhales can help your body shift out of fight-or-flight. A quick outdoor walk also helps, because changing your environment tells your brain the “threat” has passed. If your mind races at night, write a two-minute worry list, then add one next step for tomorrow. Finally, text a friend or talk to someone you trust, because social safety is powerful biology.
Don’t wait to feel calm before you act. Do the small action, and calm often follows.
Conclusion
Cortisol isn’t the enemy. It’s a helpful hormone that becomes a problem when stress and poor sleep keep it elevated. Over time, that pattern can drive cravings, belly fat, restless nights, and a slower-feeling metabolism.
Try the 14-day reset, keep it simple, and track one small metric. Give your body a few weeks of steady signals, not a weekend of perfection. If symptoms feel severe or don’t improve, get medical advice, because support beats self-blame every time.

